Pain in an emergency does not behave pleasantly. It gets here loud, typically layered, and formed by shock, fear, setting, and physiology. Handling it well is more than compassion. It is medical need. Under-treated discomfort drives tachycardia, high blood pressure, respiratory system concession, and can puzzle evaluation. The PUAEME008 Supply pain administration device sets a practical requirement for out-of-hospital responders, event medics, and scientific support staff who are anticipated to supply secure, prompt analgesia within scope. This post distills the real-world lessons behind that competency, with instances from the roadway and the resus bay, and advice relevant to any person thinking about a discomfort management training course or certification.
What PUAEME008 covers and why it matters
PUAEME008 provide pain monitoring is a nationally recognized device of expertise in Australia that prepares -responders to evaluate pain, administer approved anesthetics under professional administration, display clients, and rise when required. The emphasis gets on quick, structured analysis, risk-free medication selection, and vigilant observation, all while working within local protocols.
It complements very first -responder and pre-hospital structures by concentrating on analgesic alternatives that are practical in the area. https://rentry.co/2u3svcir Grads of a discomfort administration certification course constructed around PUAEME008 should have the ability to deliver breathed in methoxyflurane, intranasal fentanyl or comparable representatives where authorized, and non-pharmacological strategies, while documenting and connecting clearly to getting teams. For nurses and physiotherapists operating in remote clinics, sports medicine, or event coverage, the very same concepts use, and numerous discomfort management training programs integrate this device into more comprehensive ability sets.
A quick scene from practice
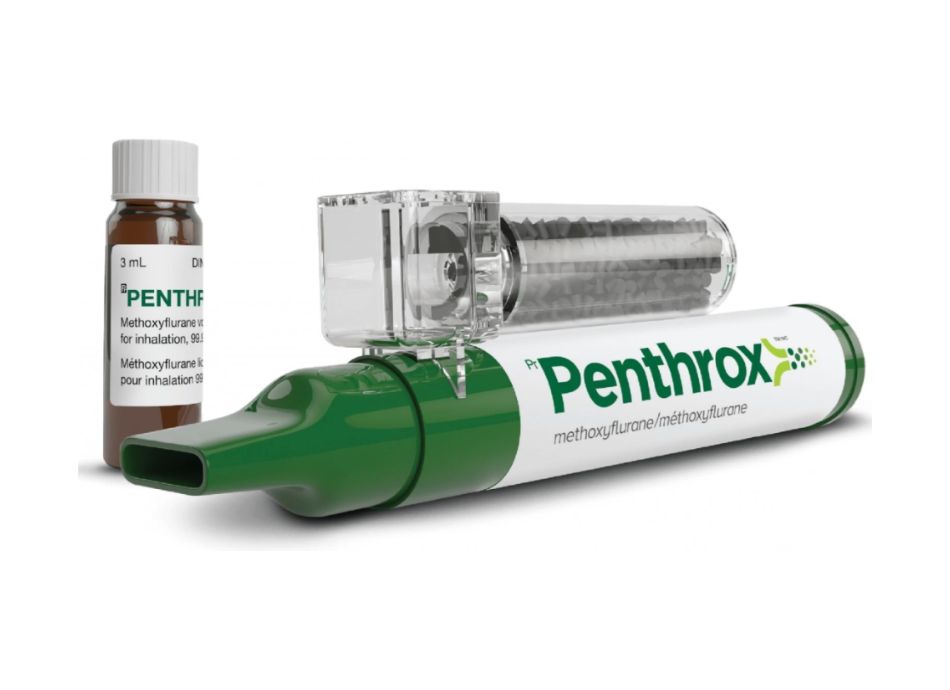
New Year's Day at a coastal occasion, a 28-year-old with a visibly warped wrist sits pale and drinking. The triage outdoor tents is humming. He rates his discomfort 9 out of 10, yet he is hyperventilating, tearful, and contradicting himself. We coach breathing, splint the arm, and deal methoxyflurane. Ten minutes later, his respirations are calmer, the hand is cozy with a palpable radial pulse, and he can respond to concerns. By the time transport gets here, we have a meaningful neurovascular assessment and clean documents. Very little tools, major difference.
The factor is straightforward. Non-pharmacological steps, combined with a quick, protocol-driven analgesic, transformed the analysis home window. PUAEME008 formalizes that sequence and minimizes the variability that comes from improvisation.
Assessment first, always
The best analgesic decision trips on an excellent analysis. In emergency situation discomfort monitoring, the assessment is quick however not superficial. I like to slow around three elements.
First, identify the discomfort. Beginning, place, radiation, top quality, and annoying aspects overview both medical diagnosis and analgesic choice. Unexpected tearing pain in the back with hypotension is not a chance for enthusiastic application; it is an aortic disaster up until tried and tested or else. Scattered stomach discomfort with securing demands warn with opioids that could cloud the photo before surgical review.
Second, measure and contextualize extent. A numerical score range is useful, yet it is not the entire tale. Look for facial grimace, protective poses, sweat, tachycardia, and the pace of speech. A stoic home builder claiming "possibly a five" while white-knuckling their upper leg should have respectful skepticism. Conversely, a very meaningful individual can report a ten yet reveal loosened up respirations and typical essential signs. Utilize both reported and observed indications, and repeat after interventions.
Third, display for warnings and contraindications. Anticoagulant use in head injury elevates the stakes. Asthma changes the discussion about NSAIDs. Background of opioid level of sensitivity, recent sedatives or alcohol, and renal impairment are not explanations. Quick checks like blood glucose can reframe agitation from discomfort to hypoglycemia. For any type of pain monitoring qualification training course, these decision factors occupy a lot of time because they are where client safety and security is won.
Weighing non-pharmacological strategies
A -responder that thinks just in milligrams misses half the toolbox. Stablizing, confidence, and fundamental strategies can go down the discomfort rating by two or 3 factors prior to a medication touches the blood stream. Hands-on experience does the convincing.
Immobilization is king for bone and joint injuries. Support the joint over and below, cushioning bony importances, and prevent over-tight bandaging that compromises perfusion. Placing issues for rib cracks and flail sectors; semi-upright with mild assistance can decrease splinting and exhaustion. For burns, get rid of the resource, cool the area with warm running water if within the initial 20 mins, after that secure from air activity which intensifies pain.
Cold and heat have their location. Acute soft tissue injuries usually resolve with ice packs wrapped, applied simply put cycles. Persistent spasm might loosen up with heat, yet in intense injury, warmth can increase bleeding. Pick intentionally and record your rationale.
Coaching breathing and attention is not fluff. Slow-moving diaphragmatic breathing slows the autonomic tornado, and a tranquil voice can anchor a worried individual enough to allow IV placement or splinting. In my experience, 60 to 90 seconds of concentrated breathing instruction while preparing an analgesic gets better end results and fewer damaging events. PUAEME008 acknowledges these steps, and good discomfort management courses bake method into scenarios.
Choosing the right analgesic in the field
Selection is an equilibrium of beginning, effectiveness, course, and side effect profile, constricted by scope and method. The common agents in pre-hospital setups have individuality quirks you find out to respect.
Methoxyflurane, a breathed in analgesic provided via a portable gadget, is quick to deploy and very titratable. It shines for moderate trauma discomfort, misplacements, and cracks throughout motion or splinting. Start is rapid, within a few breaths. Negative effects consist of wooziness and sometimes queasiness. Complete dosage limits matter due to historical nephrotoxicity worries at anesthesia-level direct exposures. Modern low-dose analgesic usage is considered secure when adhering to manufacturer restrictions and regional guidelines. Keep the gadget in the person's hand when possible so it drops away if they become sluggish. In warm settings or when dehydration is suspected, remain mindful and moisten where appropriate.
Intranasal fentanyl offers fast start without IV gain access to. It sets well with severe pain when IVs are not possible, like in combative head injury individuals or paediatrics. View breathing price and mental condition closely. Application mistakes across nostrils occur when the mucosa is crowded or blood loss. Split the dose, allow absorption, and reassess prior to offering more. Stay clear of piling several sedating agents.
Intravenous morphine and fentanyl remain staples where scope enables. Morphine's hemodynamic effects can be undesirable in hypotension. Fentanyl is cleaner in that regard, however its effectiveness needs precision and surveillance. I have seen a lot more adverse events from rush than from the drugs themselves. Slower, smaller increments with review will certainly usually defeat a large in advance dose.
Ketamine, where allowed, is a powerful ally for serious trauma pain and clients that can not endure opioids. At analgesic-dose ranges it preserves respiratory tract reflexes and spontaneous breathing. Expect dysphoria or introduction reactions periodically. A quiet, one-to-one discussion during management frequently avoids distress. Avoid in thought psychosis unless advantages strongly exceed dangers, and follow your governance to the letter.
Non-opioids should have attention. Intravenous paracetamol is underrated for moderate pain and as an opioid-sparing accessory; start is not instant, however it smooths the curve. NSAIDs can help with kidney colic or bone and joint pain provided there is no kidney disability, peptic abscess illness, or anticoagulant threat. In dehydration, skip the NSAID.
Monitoring that avoids trouble
Analgesia without monitoring is gambling. Constant or constant monitoring is the foundation of risk-free practice.
Respiratory price and top quality defeated a single SpO2 number. A tranquil 14 breaths per minute with excellent chest increase tells a various story than an irregular 8 with recurring apneas while the pulse oximeter still reveals 96 percent. Capnography, if readily available, is excellent for early discovery of hypoventilation after opioids. For intranasal fentanyl and IV opioids, repeat assessments every few mins early, then tip the frequency down once the pattern is steady.
Look beyond oxygenation. Blood pressure can wander with morphine. Heart rate usually drops as pain solves, not always as a result of negative effects. Students, level of sedation, and the client's capability to respond to a full sentence inform you whether the dosage was right. Repeat discomfort scores, yes, yet additionally note feature: can they shift setting, flex the knee, cough even more comfortably?
Good discomfort administration training courses pierce the cycle of dose, wait, reassess, document. On shift, that rhythm saves air passages and keeps groups confident.
Special populations where judgment matters
Paediatrics has a tendency to intimidate up until you have a couple of wins. Children feel much safer with a parent physically present. Intranasal paths lessen injury. Application by weight sounds apparent however is where mistakes lurk. Use color-coded aids or digital calculators if available. Observe carefully for paradoxical reactions, specifically with ketamine or benzodiazepines if your method includes them. For burns or cracks, distraction is not an incentive strategy, it is essential.
Elderly patients are extra sensitive to respiratory depressants and more likely to have comorbidities. Begin reduced, go slow, and inspect renal feature if recognized before grabbing NSAIDs. Expect ecstasy precipitated by pain, opioids, or the environment. A silent edge, glasses and hearing aids in position, and clear, low-pace descriptions can halve the confusion.
Pregnancy increases the risks. Position left lateral to prevent vena cava compression when feasible. Avoid NSAIDs in late maternity unless guided by a medical professional. Opioids may be necessary; titrate with care and involve innovative care early. Methoxyflurane use in maternity should comply with local plan and risk-benefit discussion.
Patients with persistent opioid treatment need tailored plans. Their baseline resistance frequently demands higher doses, yet resistance is not resistance to breathing clinical depression. Go for feature and relief, not total elimination of discomfort. Where feasible, verify their usual regimen and consider ketamine or regional choices if available within scope.
Speaking to extent and governance
The ideal clinicians practice well within their lane and bring help early when the roadway bends. PUAEME008 is specific regarding functioning under medical administration, regional protocols, and clinical directions. That implies you may be trained on a range of agents however authorized for a part in your solution. It also means precise paperwork, interaction with dispatch and obtaining teams, and occurrence coverage when near-misses occur.
An excellent offer pain administration course hangs around on practical administration, yet an impressive one makes you well-versed in acceleration. If you can not manage pain within your formulary, if important signs wander, or if red flags arise, you call for greater treatment. It is not a failure. It is the safety net working.
When pain covers diagnosis
Emergency medical professionals walk a line in between humane analgesia and analysis quality. The concern of "masking" can lead to undertreatment. Proof and experience reveal that suitable analgesia enhances examination high quality in many cases. You can palpate a tender abdominal area more effectively when safeguarding lowers. You can take a better background from a patient who is not panting with every word.
There are exceptions where the picture can shift. Unusual hypotension combined with severe pain needs cautious titration and immediate transportation, not duplicated dosing on scene. Believed compartment syndrome needs regular neurovascular checks and sensible analgesic use right away surgical review. For head injuries with altered mental standing, prioritize airway and neurologic tracking; provide analgesia, but keep doses traditional and view pupils and air flow closely.
Documentation that informs the story
Pain administration is as a lot a communication job as a medicinal one. Write what you saw, what you did, and what changed. Information the standard discomfort attributes, the first gauged vitals, the chosen intervention with dose, route, and time, and subsequent reassessments. Note negative impacts, the client's reported relief, and useful improvements. For handover, a clean arc of occasions constructs trust fund and guarantees continuity. In numerous services, discomfort monitoring qualification expects you to demonstrate this flow in scenarios and composed assessments.
Building competence: training that sticks
Short training courses in pain management differ. When thinking about a pain administration certificate or a pain administration qualification program, look past the brochure. Seek programs that consist of scenario-based practice with moulage, realistic time stress, and role-played communication difficulties. The most effective training strengthens decision trees for typical discussions, such as isolated limb injury, rib cracks with respiratory system splinting, kidney colic, burns, and intense back convulsion. It should instruct you to set up equipment one-handed, prime tools at night, and adjust your doses while someone is yelling for help.
For nurses and physiotherapists branching right into occasion medicine, remote centers, or sports coverage, pain monitoring training for registered nurses and discomfort administration programs for physio therapists must incorporate interprofessional communication and recommendation patterns. Knowing when to stop and intensify is as essential as recognizing how to start.

Practical suggestions that typically earn their keep
- Prepare prior to you touch the person. Draw up, examine dosages, and set tracking so the treatment really feels smooth and fast. Use the person's breath as your metronome. Coach slow breathings with methoxyflurane and observe the pattern for indicators of distress or sedation. Pair every pharmacological action with a physical one. Splint throughout onset, reposition during peak impact, safe throughout transport. Watch the second min after dosing. Damaging respiratory system patterns commonly show very early and subtly. Make your review noticeable. State the pain rating aloud, repeat the neurovascular sign in the exact same order, and reveal your partner the numbers.
These routines reduce scene times without hurrying and make groups cohesive. Pain monitoring training courses that pierce these micro-skills generate calmer clinicians.
Controlling nausea or vomiting, itching, and other side effects
Antiemetics belong when opioids or unstable analgesics cause nausea. If your method consists of ondansetron or metoclopramide, provide it early when history suggests high risk. Keep in mind liquid condition and prevent straining breakable individuals. For pruritus after opioids, confidence and time frequently are sufficient in the area; antihistamines are not always suggested and can calm unnecessarily. Constantly balance symptom treatment against the complete sedative load.
Regional and progressed options
Many out-of-hospital carriers do not do nerve blocks, however some advanced teams and remote clinicians do. Femoral nerve blocks for hip cracks can change care. If your range includes them, value the prep work: sterilized strategy, ultrasound where feasible, and careful dosing. When not available, a well-applied traction splint and systemic analgesia stay effective. For rib fractures, devoted splinting and targeted breathing mentoring can decrease the need for high opioid doses. Regional choices deserve comprehending even if you can not do them; they affect your handover and your pre-transport plan.
The emotional layer
Pain is never purely physical. Injury scenes come with worry, guilt, and in some cases embarassment. A few sentences of validation minimize suffering in quantifiable ways. "Your leg is damaged. The discomfort you feel makes sense. We are providing you medicine that works swiftly. You are risk-free now." This is not bedside fluff. It reduces catecholamines, enhances participation, and lowers the dosage you need. For patients with a history of substance use, a neutral, considerate tone prevents preconception. Record neutrally and focus on the physiology and response.
Learning from mistakes without making them twice
Every experienced medical professional can recall a time they under-treated out of care, or stacked agents too promptly under pressure. The remedy is calculated method and debrief. After a difficult instance, ask three questions. What did we discover late? Where did we rush? What would we transform with the same constraints? Motivate your group to maintain a brief representation log. Over a year, those notes build a personal certificate training course suffering administration better than any type of classroom handout.
Choosing the appropriate program pathway
If you are taking into consideration official training, match the offer to your duty. For event medics and first -responders, a give pain monitoring training course straightened to PUAEME008 will concentrate on breathed in and intranasal options, circumstance drills, and documentation. For clinicians seeking a wider discomfort monitoring certification, try to find programs that include severe and persistent frameworks, pharmacology refresher courses, and legal elements of providing Set up 8 drugs within your jurisdiction.
Pain monitoring training courses for nurses who work in emergency situation departments or urgent care should emphasize triage analgesia, fast-track paths for fractures, and pain management certificate workshops paediatric dosing, in addition to protocolized antiemetic use and rise. Pain administration training courses for physiotherapists can include acute injury inflection strategies, taping and supporting during the acute home window, and partnership with prescribers for consolidated methods. Brief programs in pain management can be powerful if they are practical, hands-on, and include follow-up technique or assessments.
Logistics that maintain kits ready
Good analgesia stops working when the container is empty or the atomizer is missing. Develop a checklist culture. For teams covering occasions, stock one secured pain kit per -responder and one book in the command post. Turn short-expiry items to clinical bases prior to they pass their dates. Keep created dose charts laminated flooring, not buried in a phone with a dead battery. Tag atomizers and syringes by quantity provided per milliliter to minimize head math. For methoxyflurane, shop devices out of direct sun and inform staff on filter changes and device disposal.
Working within the law and ethics
Administering analgesics in the area includes legal responsibilities. Follow your service's consent matrix for Schedule 2, 3, 4, or 8 medications. Safe and secure storage space, temperature level controls where needed, and paperwork of waste are non-negotiable. Consent matters also suffering. In the slightly overwhelmed client that resists, focus on non-pharmacological procedures and transport. For minors, look for guardian authorization when possible; in emergencies, suggested consent applies, but interact your activities plainly and early.
Ethically, treat discomfort equitably. Older grownups, people with communication obstacles, and those with mental health histories are at risk of under-treatment. Structured analyses close the space. At the exact same time, be wise with repeat calls from familiar addresses. Deal with the instant issue, check for red flags, and coordinate with wider care networks as opposed to drifting right into without supervision chronic discomfort management.
Bringing it all with each other on a busy shift
Picture a two-hour stretch on a Saturday: a wrist crack at a football ground, a renal colic phone call to a small flat, and a bicyclist with rib cracks after a low-speed bus encounter. Three different pains, 3 different moods. The first gets methoxyflurane, a reassuring presence, and a thoughtful splint. The 2nd benefits from intranasal fentanyl after mentoring and hydration recommendations, with a prepare for ED imaging. The 3rd demands mindful respiratory system assessment, step-by-step fentanyl with capnography, a pillow support to cough, and instructions to deep breathe every couple of mins heading in. Each instance uses the exact same map: evaluate, select, provide, monitor, reassess, record, and turn over. The details differ. The technique does not.
PUAEME008 offer pain monitoring gives that self-control an usual language throughout solutions. For teams that embrace it, brand-new staff join a discussion currently in progress. The unit will certainly not replace clinical judgment, but it will certainly hone it, particularly under pressure.
Final ideas for medical professionals considering training
If you lug obligation for clients in sharp pain, invest in structured training. A pain administration certification rooted in reasonable situations will increase your ceiling and your floor. Select a company that values your extent and context, whether you are a first -responder, a registered nurse in a rural immediate treatment facility, or a physiotherapist covering an exclusive sports satisfy. Anticipate to exercise up until the series feels like muscular tissue memory. Anticipate responses that stings a little. Expect less poor changes and much better handovers.
Pain is unpreventable. Experiencing is not. With disciplined analysis, pragmatic methods, and the appropriate education and learning, you can lift people out of the panic and into a room where diagnostics, transport, and healing continue smoothly. That is the pledge behind top quality discomfort administration training and the everyday craft of emergency care.